Meet The Man Who Stopped Thousands Of People Becoming HIV-Positive
“I knew I was doing something of substance, but it’s really
overwhelming.” In an exclusive interview with BuzzFeed News, Greg Owen
reveals the story behind Britain’s largest ever drop in HIV
transmissions.
One of the world’s most esteemed HIV doctors, Professor Sheena McCormack – whose life’s work as an epidemiologist has been to track and fight the virus – picked up the phone to deliver a message that would make headline news: In the space of 12 months, the number of gay men in London being diagnosed with HIV had dropped by 40%. Across England it was down by a third.
No British doctor has been able to report a fall this steep in more than 35 years of the virus. It is the kind of figure that in medical circles is so large as to look jarring, even false; and yet it was true.
Behind this story lay a series of secret meetings and a network of people with one man at the centre who, unknown to the public, helped change medical history. His name is Greg Owen. He was the man McCormack phoned. Today his story is told in full for the first time.

“She said, ‘Don’t look at the percentage; I want you to look at this another way. There are thousands of people who didn’t become HIV-positive this year because of you.’”
Owen started to cry. And after that call, he says, he used to cry every day.
“I knew I was doing something of substance, but I didn’t know what. It feels really good but it’s really overwhelming because how many people in my position get to do what I did?”
The man McCormack credited with this unprecedented reduction in HIV transmissions was not a fellow doctor, nor the head of a charity, nor even a politician. Owen is unemployed, a former sex worker, and homeless.
What he managed to pull off – and why – is so outlandish it warrants comparisons with Ron Woodroof, the AIDS patient depicted by Matthew McConaughey in Dallas Buyers Club, who in 1980s America smuggled in unauthorised HIV drugs for desperate fellow sufferers.
The difference is that Woodroof’s was an outrageous story that ended in tragedy. Owen’s is a tragic story that ends in outrageous success.

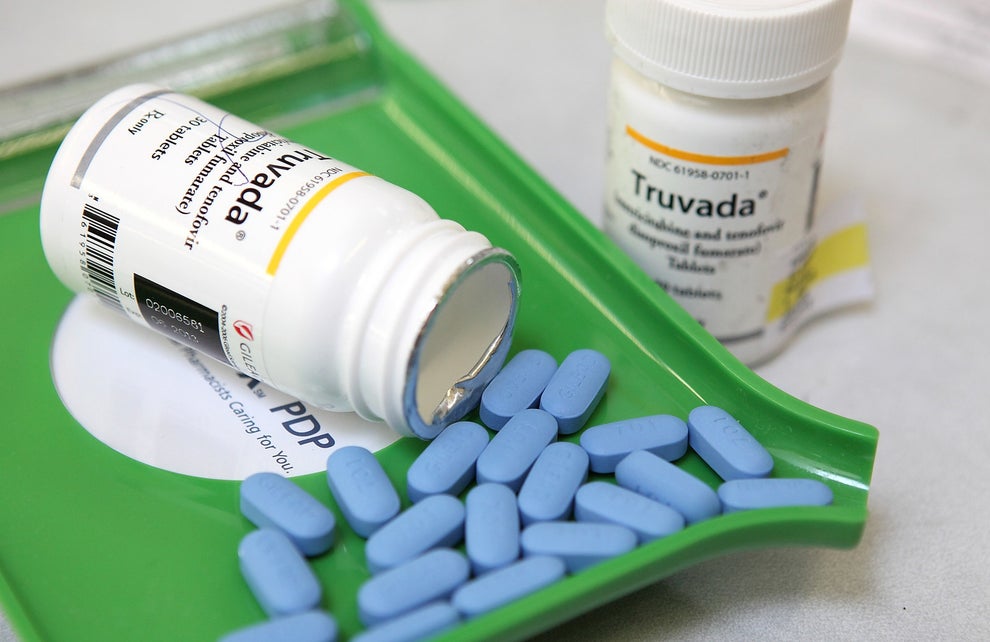
Justin Sullivan / Getty Images
He had heard about a new drug regime that was being used to prevent HIV. The medication’s brand name is Truvada, and the regime – which involves taking this antiretroviral pill every day – is dubbed PrEP: pre-exposure prophylaxis. Owen, fearful of contracting the virus amid this unleashed world, couldn’t decide whether to start taking the drug, let alone how to obtain it.
PrEP was not available on the NHS and a private prescription would cost about £500 per month. But a major NHS study was underway to ascertain how effective the drug was, and who should be given it. The study, called PROUD, was being run by Professor McCormack.
“I heard about the PROUD study at a sex party,” says Owen, casually, in the middle of a much longer sentence. He talks at twice the speed of most people, with clauses within clauses and tangents branching from other tangents in a bewildering cascade of verbal Russian dolls.
The problem was that Owen was too late to enrol in the study. He was also increasingly aware of his own chaotic situation: After a relationship breakdown and a suicide attempt, Owen was sleeping on friends’ sofas and sliding into full escapism mode.
“I’d gone through enough risk-taking,” he says in his soft Belfast accent. “I was like, ‘You know what? I just need to do this – I take GHB and smoke crystal [meth] all weekend.’”
But there was another reason for Owen’s determination. He had watched someone he loved (who we cannot name in order to protect their anonymity) fall apart after being diagnosed.
“He was in a really bad state,” says Owen. The man descended so far into the drugs scene in an attempt to blot out the diagnosis that he had had a heart attack soon after. “He was having a breakdown. Everything was fucked.”
After trying in vain to help him, Owen focused on remaining HIV-negative himself and seeing if there was some way to help HIV-positive people more generally.
On 11 August 2015, Owen posted on Facebook to let his friends know that he planned to begin taking PrEP. A friend, who was HIV-positive and had been prescribed the drug as part of his treatment before switching medication, offered him some spare pills. Owen’s plan was to start taking them and blog about his experiences – a “blow by blow” account, he says, laughing. Owen laughs a lot when he isn’t raging, frowning, or grinning with delight – often with a frenzy of gestures. He is rarely still.

Laura Gallant / BuzzFeed
“I felt sick,” says Owen. “I said, ‘I need to have a cigarette.’ I was in shock.”
The following evening, aware that his friends on Facebook would soon be asking how he was getting on with PrEP, and while working a shift in a gay bar, Owen posted an update on the site telling everyone he was HIV-positive.
That single act triggered a chain of events that would change everything.
“When I came out on my break two hours later, I had 375 likes, 175 comments, 50 shares. I was like, ‘Sweet Jesus,’” he says. “Then I opened my Messenger – streams of disclosures and supportive messages from people. I must have had 50 or 60 people in two hours saying, ‘I can’t believe you’ve done that, I’m HIV-positive as well and I haven’t told anyone,’ or, ‘I have only told my family and you’ve told 5,000 people.’”
But then the messages started changing. “People were like, ‘What is this PrEP thing and if you had it why wouldn’t you have become HIV-positive?’ It got to a point within a week where I would get 10 people a day asking me about PrEP – and that’s 10 people asking 10 questions each.”
Keen to get on with life and with his blog, Owen found the questions from acquaintances and strangers were proving a near-constant interruption. He told his friend Alex that something had to give. And it was then that he remembered something.
“I was like, ‘I’m sure I was at a meeting somewhere and heard you can import generic hepatitis C drugs for a tenth of the price,’” he says. This thought fused with the need to rid himself of the endless inquiries, or “these fucking bastards asking me about PrEP”, as he puts it.
He decided to set up a website with all the information he could find, thus allowing him to “walk away from PrEP”. He laughs at the irony. It would prove to do the opposite. The idea for the site wasn’t only to provide facts; it was also going to help readers buy cheap, non-branded versions of the drug – known as “generics” – from manufacturers overseas.

“I said, ‘I’m aware we can maybe import something? Do you know anything about this?’ And he replied, ‘Yeeeeees. Come in tomorrow at 3pm.’”
The next day they met in the clinic. Owen was told to keep everything confidential.
“This person said, ‘We have a handful of people who use our clinic and they have been self-sourcing generics from this website and we have been discreetly doing the monitoring – discreetly checking their blood periodically to check that there’s active levels of the drug.’”
In one sentence, everything was possible. There was somewhere to buy the non-branded versions of the drug – and at around £50 a month, a tenth of the price of a private prescription. And there was, potentially, a way to ensure the drugs were working properly. At the time, because PrEP was not available on the NHS, neither – officially – were the urine and blood tests needed to check that the drugs were not adversely affecting kidney function (which some antiretrovirals can do) and were not fake.
The man in the clinic, says Owen, then made the possible workable: He showed Owen which websites were supplying this handful of patients with the generics, and which ones they knew – because they had run the tests – were supplying the effective pills.
“I said, ‘So this is legit – legit but dodgy. Can we do this?’ And he said, ‘Not only can you do this; you must do this. We’ve been waiting for someone to do this. We’re diagnosing people every day and do you know how heart-breaking it is to know that PrEP would stop it and not be able to do something?’”
And that, says Owen, was all the motivation he needed. He and his friend Alex spent a few weeks building the website, gathering as much information as they could, and including a simple click-to-buy button that linked through to the pharmacies in Asia that sold and shipped the generics. They called it IWantPrEPNow.co.uk.
“At the time I was shitting myself,” he says. “I was thinking, ‘It’s not like I’m selling Viagra that might work or might not work – the worst that happens is you don’t get a boner – I’m selling drugs where people might rely on it for their HIV protection.”
But by then, September 2015, the results of the PROUD study were in: PrEP was enormously effective – comparable to condoms – but unlike condoms, this pill is not reliant on people being able or willing to implement the precaution at the very moment when desire can overwhelm. Add in drugs or alcohol, low self-esteem or even self-destruction, and the underuse of condoms across all demographics is hardly surprising. PrEP offered a viable alternative.


No comments:
Post a Comment